260 – Canine Cognitive Dysfunction is More Than Old Age
Canine Cognitive Dysfunction is More Than Old Age
Dr. Marty Greer, DVM is back with this month’s Veterinary Voice topic, Canine Cognitive Dysfunction.
Canine Cognitive Dysfunction/Cognitive Dysfunction Syndrome: (CDS) is a neurobehavioral disorder affecting geriatric dogs and cats that is characterized by an age-related decline in cognitive abilities sufficient to affect functioning, with behavior changes that are not attributable to other medical conditions.
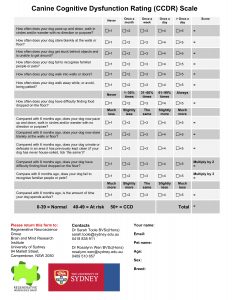 Signs of Dog Dementia
Signs of Dog Dementia
To look out for canine cognitive dysfunction, remember to check your dog’s “DISH”:
- Disorientation
- Paces
- Wanders aimlessly
- Becomes stuck on the wrong side of the door or behind furniture
- Staring at walls or into space
- Seems lost in the yard or forgets the purpose of going outside
- Forgets where the water and food bowls and doors are
- Fails to recognize familiar people or dogs
- Reduced responsiveness to name or verbal commands
- Abnormal response – increased or decreased – to familiar objects
- Difficulty learning new tasks
- Difficulty performing previously learned task
- Loss of interest in food
- Repetitive behaviors
- Interaction with Family Members
- Seeks less attention (petting, belly rubs, play)
- Less enthusiastic to greet people or other pets in the home
- No longer greets family upon arriving home
- Fails to respond to verbal cues
- Increased irritability and/or aggression with family and pets
- Changes in exploratory behavior
- Intolerant of being left alone
- Sleep and Activity
- Sleeps more hours per day, especially during the daytime
- Sleeps less throughout the night
- Reduced daily activity
- Lack of interest in his surroundings
- Restlessness, pacing, wandering or circling at sunset (sundowning)
- Vocalization at night (barking or howling)
- House Training
- Urinates or defecates indoors
- Urinates or defecates indoors soon after having been outside
- Failure to indicate need to go outside
- Accidents occur in front of his owners
- Elimination at uncommon outdoor locations such as on concrete
Cause
The neuroanatomic pathology in dogs and cats shares some characteristics with human Alzheimer’s disease, specifically β-amyloid accumulation, tau phosphorylation and neuronal loss in the frontal cortex, cerebellum, and hippocampus.
Managing Canine Cognitive Dysfunction
- Purina Neurocare/Bright Minds
- Hills B/D
- Royal canin
- Addition of antioxidants (Vitamin C and E) for cellular-level health and medium-chain triglycerides for cognitive improvement. L-Carnitine for muscle mass.
- Phosphatidylserine, Apoaequorin and S-Adenosyl-l-Methionine (SAME)
- Anipryl/selegeline – Is a selective monoamine oxidase -B inhibitor, which could enhance catecholamine neuron activity and increases dopamine levels in dogs.
- DHA
- Avoid unnecessary vaccines
- Skip pharmaceuticals when possible
- Reduce stress including changes in their routine and environment
- Potty pads, confinement, outside more often
- Pet-proof the house
- Social interaction and mental engagement/ environmental enrichment
- Keep the day/night cycles regular with sunlight
- Walking/exercise/stroller if needed
- Situational anti-anxiety drugs – trazodone and gabapentin
250 – Veterinary Voice: Prostate Problems, Prevention and Solutions
Prostate Problems, Prevention and Solutions
Dr. Marty Greer gives us the low down on male dog prostate and reproductive issues. Additional discussion on emergency semen collection, dogs whose semen doesn’t extend well and more.
“This is an area that is often misunderstood by the general practitioner vet,” Greer said.
Symptoms
Symptoms of a prostatic complication include blood in the urine or ejaculate, straining to pass stool, blood dripping from the penis, Greer added.
Diagnosis
Prostate cancer, benign prostatic hypertrophy, prostatitis are the most common complications. Dogs over five years old are the most commonly affected.
Greer advises that neutering is not absolutely necessary for dogs with non-cancerous prostate disease.
Dogs with a prostate infection are very sick, typically run a fever and clearly don’t feel well, Greer said.
Prostatic cancer manifests in two different forms. Which type the dog has needs to be confirmed with a biopsy.
“Both kinds of prostate cancer are quite serious,” Greer said. “Counterintuitively, it is almost always a neutered dog that has these cancers.”
Treatment
Benign prostatic hypertrophy (enlarged prostate) is a hormonal disease, Greer noted. Dogs don’t need antibiotics, neutering isn’t required. The condition can be successfully treated with hormone therapy.
“Neutering will cure BPH and prostatitis. However, it is very difficult to breed neutered male dogs, unless they have had semen frozen. The best time to freeze semen is when a dog is between 2 and 5 years of age. The dog should be healthy and producing great quality semen. It will cost you a lot less money to freeze a canine’s semen when he is young. If he later turns out to have a disorder that you don’t want in your breeding program, you can either wait until a DNA test is conducted to determine how you can use him in your breeding program or discard the semen.” — Dr. Marty Greer
242 – Veterinary Voice: K9 Flu and Puppy Vaccination Protocols
K9 Flu Is Serious Risk Because Dogs Have No Natural Immunity
Dr. Marty Greer takes us through the outbreaks of Canine Influenza (K9 Flu) in the United States. She also offers recommended vaccination protocols for adults and puppies.
Outbreaks of two different strains of Canine Influenza have left U.S. dog owners struggling with if and when to vaccinate against this virus. Greer advocates strongly for “yes” and “annually.”
K9 Flu causes pneumonia
“No dogs have natural immunity to the disease,” Greer said. “Unless vaccinated, dogs are at serious risk. I have my personal dogs on a three-year protocol, but even Dr. Ronald Schultz is advocating that owners vaccinate for influenza in ALL dogs.”
Greer notes that the 2015 virus outbreak came with Korean meat dog “rescue” imports and spread rapidly. Dogs traveling for competition at the highest risk of contact.
Influenza in the dog causes pneumonia, Greer said. The symptoms look like kennel cough to start, but progress rapidly to pneumonia, including a hemorrhagic variant.
“Eight percent of infected dogs die,” Greer said. “This really is a big deal.”
An ounce of prevention is worth a pound of cure
Treatment with two weeks of antibiotics, iv fluids, possibly even oxygen, is common Greer said. Follow up xrays to confirm the pneumonia is controlled are required. Even dogs less severely affected are infectious for up to 3 weeks.
Two vaccine companies offer products which cover both strains of the disease and are readily available, Greer said. The vaccinations require two injections, two-four weeks apart, with an annual booster. Since the vaccines have only been available since 2016, there isn’t sufficient data to determine if they are effective longer than that.
Impacts on puppy vaccination protocols
Adding the K9 Flu vaccine into a puppy vaccination protocol can be a challenge, but Greer said the vaccine can be given as young as seven weeks of age. She recommends inoculating on a staggered schedule. She also strongly recommends the nomograph system of establishing vaccination timing for puppies. Her recommendation is to pull blood on the dam at the same appointment in which ultrasound confirms pregnancy. This blood is shipped off to a laboratory that measures the bitch’s immunity levels to disease and pinpoints exactly what date the puppies should be vaccinated.
Canine Nomograph – What is it?
A nomograph is an estimate of the amount of antibody passed to a litter of pups from the mother via her colostrum. During the puppy’s first hours of life, its intestinal tract is able to allow colostral antibody to be absorbed into the bloodstream. This passive antibody helps to protect the newborn from all the diseases that the mother is protected from. As the puppy grows up, maternal antibody breaks down in approximately 2 week “half lives” until it is no longer present in the pup. While this antibody is at higher levels, it is able to neutralize viruses such as canine parvovirus and canine distemper virus. Because of this neutralization, puppy vaccine can be blocked. Maternal antibody interference is one of the most common causes of vaccine failure to immunize! The reason that puppies are given multiple doses of vaccine is because most of the time we don’t know what their maternal antibody titers are, and so don’t know when the vaccine will be effective. Nomograph testing helps us understand the best timing of vaccination to assure a litter will be effectively immunized. Because the nomograph is limited by the ability of the dam to make colostrum and for the pups to receive it, nomograph results should not be used as a definitive indication of protection from disease. If you are a breeder who is experiencing a disease outbreak, please contact us prior to submitting a nomograph.
(Reference: Baker, Robson, Gillespie, Burgher, and Doughty. A nomograph that predicts the age to vaccinate puppies against distemper. Cornell Veterinarian, Aug 1958, page 158-167.)
Listen to Dr. Gayle Watkins in an early PureDogTalk interview on the topic of nomographs.
224 — Veterinary Voice: Pyometra is an Emergency
Pyometra is a life threatening disease
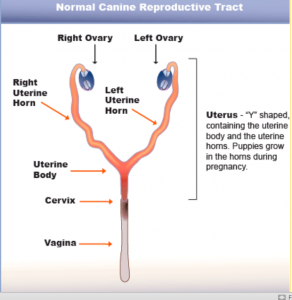 Pyometra is a severe bacterial infection with accumulation of pus within the uterus. Though it often occurs with middle-aged or older unspayed females, younger dogs are sometimes affected. Pyometra most commonly develops a few weeks after a heat cycle. The condition results from hormonal changes that decrease the normal resistance to infection. As a result, bacteria enter the fluid in the uterus and large volumes of pus can accumulate.
Pyometra is a severe bacterial infection with accumulation of pus within the uterus. Though it often occurs with middle-aged or older unspayed females, younger dogs are sometimes affected. Pyometra most commonly develops a few weeks after a heat cycle. The condition results from hormonal changes that decrease the normal resistance to infection. As a result, bacteria enter the fluid in the uterus and large volumes of pus can accumulate.
Signs of Pyometra include loss of appetite, excessive thirst and urination, lethargy, and/or vomiting. Sometimes, there is a vaginal discharge. The disease may develop very slowly over several weeks.
This condition often requires emergency surgery, provided the animal is stable. Surgery consists of removing both ovaries and uterus, which not only corrects the condition, but also eliminates bothersome heat cycles. Because the patient is ill and the uterus is infected, the surgery is more complicated and carries a higher risk than a routine spay. Ultrasound and blood tests are useful in both diagnosing and evaluating surgical risk. Post-operative treatment includes antibiotics and intravenous fluids.
For dogs who are in a breeding program, Dr. Marty Greer, DVM provides information in the podcast about medical management that may avoid the spay surgery.
Pyometra
From Dr. Greer…. “Your pet has presented with a condition called pyometra, or a uterine infection. These can be life-threatening, and most cases will not resolve without surgery. Pyometra usually occurs 1-5 weeks after the last heat cycle. In this illness, the uterus has filled up with pus (white blood cells and bacteria) and is at risk for rupturing if not treated immediately.
Prior to surgery, we will stabilize your pet with intravenous fluids, antibiotics, and pain medications. Most patients with pyometra are very sick – with either a very high or very low white blood cell count, fever, dehydration, a low blood sugar, and vomiting and diarrhea. As soon as your pet is able to tolerate anesthesia, we will start surgery to remove the uterus.
Your pet will be in the hospital for at least 2-5 days, depending on how she does during surgery and afterwards. It is important to know the possible complications of pyometra surgery. These include:
- Peritonitis is the most common. This means infection within the abdomen. It is treated with antibiotics, IV fluids, and may require additional surgery and drainage.
- Rupture of uterus in surgery. The uterus is often very thin and easily damaged. It is possible that it can rupture during surgery, spilling pus into the abdomen. This can prolong the hospitalization for several days.
- Aspiration pneumonia. Fluid and food sometimes bubble up into the throat and mouth during surgery. This can be inhaled into the lungs, leading to pneumonia. Every precaution is taken to avoid this, but it still happens in some cases.
- Sepsis, systemic inflammatory response syndrome, acute respiratory distress syndrome (ARDS), and disseminated intravascular coagulation can also occur before, during, or after surgery. These are uncommon complications in which the white blood cell count drops, the patient develops or continues to have a fever, sometimes develops difficulty breathing and difficulty with normal blood clotting. These are not common but can occur. If they do, very aggressive treatment must be undertaken to save your pet and can significantly prolong hospitalization and lead to death.
- Acute kidney failure can occur before, during, or after surgery. This is not a common complication but can happen. Often patients will also have a urinary tract infection. Once your pet is stable, eating, comfortable and able to take oral medications, discharge home can be discussed with the doctor. ”
216 — Vet Voice: Blastomycosis and Other Fungal Infections
Blastomycosis is deadly hazard for dogs
Dr. Marty Greer, DVM, discusses the causes, symptoms and treatment of deadly Blastomycosis and other fungal infections. Greer notes that fully 25 percent of dogs affected by this disease will die.
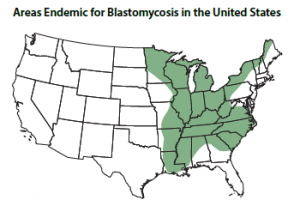
Greer is notably not an alarmist, but she is adamant that Blastomycosis is a deadly and dangerous disease. Specific areas of the country, including the upper Midwest and South/East River valleys, are most commonly affected.
This particular fungal infection is contracted by spores inhaled from disrupted soil, particularly near water. Greer also addresses other fungal infections that can affect dogs.
The most common symptom of Blastomycosis is a dog that is coughing, sounding like pneumonia. The dogs will often also present with a draining sore on the foot that is of indeterminate cause.
Diagnostics for the disease are conducted on urine samples sent to a specific laboratory in Indiana. Dogs can decline rapidly, with acute onset of the disease in less than 24 hours. Treatment of the disease is expensive, time consuming and even successful treatment may leave the dog with permanent damage.
Dogs are treated with oral medication, with a 75 to 90 percent success rate, using the urine test to monitor efficacy of treatment.
Zoonotic disease
Blastomycosis is a zoonotic disease, meaning it affects people and animals. People will not be exposed by their sick dogs, but they can acquire the disease from the same source of disrupted soil. The spores live in the soil. She goes so far as to recommend dogs that pass from the disease be cremated, not buried, so as to not release more spores into the soil.
“There have been outbreaks where 120 people were sickened in one event,” Greer said. “It is bad, bad stuff. Nobody messes around with this. It is serious.”
Blasto can be a challenge to diagnose, as the early symptoms are similar to many other diseases, Greer said. She adds that owners should keep track of dogs after traveling to areas where the disease is prevalent.
198 – Vet Voice: Dog Days of Summer Precautions
Dog Days of Summer Precautions
Dr. Marty Greer, DVM takes us through a few summer dangers, how to avoid them and some excellent tricks to solve some of them. Listen to find out why canned spinach and Dawn dish soap are on her “must have” list.
Hot cars
“Nobody leaves a dog in the car on purpose,” Greer said. “They get distracted and lose track of time.” She recommends keeping a leash draped around your neck as a simple reminder. And to never trust the AC in a running car.
Leave a note on the car’s dash with your cel phone number in those instances when you need to make a quick dash inside a store, Greer suggested, so people won’t try to ‘rescue’ a dog that doesn’t need it or in case of actual emergency.
Blue-green algae
These toxic algae blooms in still water are not common, Greer said, but they are dangerous. She recommends keeping Dawn dish soap on hand to wash a dog that has been in questionable water. And not allowing dogs to drink water that is not free running and clear
Canned spinach??
Greer said this easy, cheap household staple can be fed to dogs who have consumed small, sharp objects that could cause gastrointestinal distress like sharp bones from a barbecue.
“The spinach wraps itself around the item and allows the dogs to safely pass small sharp items,” Greer said. “Every year we have dogs that don’t have to go to surgery thanks to this — diamond rings, you name it.”
Cookouts and holiday festivities are always of concern with our dogs. She noted that corn cobs are a particularly common source of bowel obstruction.
Foxtails
These nasty weed seeds are deadly dangerous to our dogs. They can penetrate skin and migrate anywhere. Commonly they become imbedded between a dog’s pads. In the best case scenario, the seeds simply abscess and make a lame dog. Seeds can get in the dog’s ear, working their way down to puncture the ear drum and cause painful ear infections. Worst case, Greer noted, is when foxtails travel to the lungs from the nose, or even feet, and cause a pneumothorax. Saving the dog’s life then requires dangerous and extremely costly surgery.
Greer recommends prevention by checking your dog after every outing in the field and learning to recognize the dangerous plants by visiting http://www.meanseeds.com/, a website created by a client of hers in Wisconsin.
Ticks
“These are nasty creatures we want to avoid,” Greer said. “Changes in climate have impacted the spread of ticks.”
An ounce of prevention, again, is worth a pound cure. Greer suggests that dogs be on flea/tick preventative year-round and that the current products are safe and effective. She is happy to provide current information about products that are safe to use with dogs in a breeding program. Visit https://www.smallanimalclinic.com/ for more information.
Ticks are vectors for zoonotic diseases including Lyme’s, anaplasmosis, Ehrlichia, Rocky Mountain Spotted Fever and potentially dozens more that as yet are unidentified, Greer noted.
“There are new diseases, even new ticks,” Greer said. “It’s startling how many tick borne diseases out there.” She recommends visiting https://www.capcvet.org/ for more information
Canine flu
Greer’s advice: “Vaccinate. Any dogs in competitive venues or that even leave their houses should be vaccinated. There is no natural immunity in the population because these are new viruses.”
Thunderstorms/fireworks
Talk to your vet about anti-anxiety meds, Greer said. Acepromazine and Benadryl are not anti-anxiety drugs, they just make the dog unable to show you how scared they are, she added.
190 – Leptospirosis symptoms, treatments and prevention

Dr. Marty Greer
Leptospirosis symptoms, treatments and prevention
Dr. Marty Greer, DVM, JD joins us again for our monthly Veterinary Voice. Our topic this month is the potentially deadly zoonotic disease, leptospirosis.
Resurgent disease
Aka Lepto, this bacterial infection is found primarily in areas of standing water and within about 18 months of major flooding. Desert and dry regions see very little of the disease. Greer said the veterinary community is seeing a resurgence in this dangerous infection.
A spirochete bacteria, Lepto looks like a corkscrew under a microscope. The actual physical shape of the bug is instrumental in how it impacts the host. These little creatures burrow into tissue, primarily in the liver and kidney. They can frequently live *undetected* in the host for years. The germs are shed in the urine of affected animals.
Lepto bacteria are transmitted through mucus membranes. Livestock and wildlife are the primary points of exposure for our dogs. Pets who trot out to do their business and investigate overnight visitors in the yard are at risk just as much as hunting dogs.
Symptoms
This is a zoonotic disease (communicable to humans as well as animals) which may cause any and or all of the following symptoms in our pets:
- Drink more,
- urinate more,
- vomiting,
- diarrhea,
- maybe even a cough….
- High liver enzymes and high kidney values on same blood panel…
- fever,
- lethargic,
- jaundice (yellow),
- lower appetite,
- stiff/painful…
“The problem is, these symptoms are common to other diseases,” Greer said. “The dogs can be asymptomatic to critically ill.”
Prevention
Greer advocates for a three-year vaccine protocol for viral diseases like distemper and parvo. But she strongly encourages her clients to incorporate a one-year plan for the bacterial diseases such as leptospirosis and bordatella.
“We see (lepto) primarily in the spring and fall,” Greer said. “But you have to test specifically for it to know for sure what’s going on. The vaccines we have available today are safer and far more effective than they were 10-15 years ago,” making them far less likely to cause a vaccine reaction and more likely to prevent all of the strains of the disease.
Diagnosis
Lepto can be diagnosed specifically only with a DNA test drawn from urine when the dog is acutely sick. This test seeks to identify the actual DNA of the bacteria. A blood test also can determine titers for lepto. What this titer seeks is to look for the actual disease instead of *immunity* to the disease through vaccination.
Treatment
Greer said an ultrasound to determine kidney/liver involvement can be needed. And antibiotics, either doxycycline and/or amoxicillin, may be prescribed.
Since lepto can be asymptomatic and can spread quickly to remaining dogs (and children or adults) in a kennel/household, proper diagnosis, prevention or treatment are imperative.
Greer recommends this vaccination guideline (link below) to help determine what a dog may or may not need for the specific lifestyle it pursues.
https://www.aaha.org/pet_owner/aaha_guidelines/aahas_canine_vaccination_guidelines.aspx
180 – Veterinary Voice: Dr. Marty Greer Talks “Frozen Assets”
Dr. Marty Greer Talks “Frozen Assets”
Frozen semen is an investment not only in one family of dogs, but in the future of the breed in question. Dr. Marty Greer, DVM, JD takes us through a checklist of important considerations for preserving genetic material from our best dogs.
First, Greer said, be sure the semen is stored in a safe facility. Sometimes even storing the same dog’s semen in more than one facility is worth the cost.
Greer’s story about a private semen storage whose owner passed away without a will in place is a cautionary tale.
Insure the Future with Frozen Semen
Second, make provisions for transfer of semen ownership, whether in a will or trust, Greer said. This vital step will ensure the safety of valuable genetics.
“Don’t look at it as your dog line’s future,” Greer said, “but take a step back and look at it as the future of your breed.”
She contends the value of frozen semen is that the best dogs are what we have in frozen. Improvement in testing for diseases means we can use genetic material even if it is imperfect, by using DNA testing to line up the frozen semen with an appropriate bitch.
“If we can test their semen … they’ve got preserved,” Greer said “and use those to match with the appropriate bitches, we can really move our breeds forward, if we’re willing to think hard about this and not just be looking at that little tiny bit of your genetic material but look at your breed as a whole …”
Greer is a strong advocate for planning ahead for the transferal of frozen semen ownership. And to consider sharing it outside one’s own breeding program.
“And in our semen freezing contracts we have a provision made for how that semen should be transferred,” Greer said. “You should have it in your will. You should talk to your attorney about it and a lot of attorneys are going to be unfamiliar with this kind of transaction. So you’re probably going to want to talk to somebody that has some expertise. Somebody in a legal position that they’ve either got a dog ownership and they’re attorneys as well. Debra Hamilton does a lot of work with trust for dogs.”
Another point Greer makes is acquiring insurance for the storage of the semen.
“ I have a few clients that have purchased old semen from their mentors,” Greer said “and they may have 10 to 20 dogs frozen and so they may have a good deal of financial investment in that. … insurance is available through a small number of companies but don’t count on it being insured at the place that you’re storing it.”
Greer also provides input on how to estimate fair charges for owners who will sell vials of frozen semen to other breeders.
Listen today for all of Greer’s great advice.
And if you missed it, you can listen to our interview last summer with Debra Hamilton on the topic of creating plans for the future of your dogs, breeding program and more at this link: https://puredogtalk.com/96-divorce-disease-disaster-disability-delay-death-and-your-dogs-debra-hamilton-esq-how-to-make-a-maap-plan-2/
162 – Veterinary Voice: Health Testing 101 with Dr. Marty Greer
VETERINARY VOICE: HEALTH TESTING 101 – DR. MARTY GREER
Dr. Marty Greer, DVM, JD returns to our Veterinary Voice series to talk about health testing for our breeding programs.
Using testing to improve our dogs’ overall health involves looking at both “phenotype” — diseases we can test for with xrays, blood or other physical exam — and “genotype” — those diseases identified by DNA testing.
Dr. Greer also provides some great input on the various DNA tests cropping up all around us. These tests, all spinning off from the identification of the canine genome, provide breeders, exhibitors and pet owners with a plethora of options for naming everything from the mixture of breeds in a shelter dog to the specific heritable genes for deadly diseases.
One of Greer’s primary points, which we’ll touch on again next week in our podcast with Dr. Jerold Bell, is that these health testing options provide breeders with the ability to *expand* their gene pools. Scientifically identifying a dog as a carrier and another as a non-carrier of a specific disease gene, for example, enables breeders to breed those two individuals with the assurance that none of the resulting progeny will be affected by the disease in question.
Many of our dogs are impacted by polygenic diseases, in other words something like hip dysplasia, for which there is no DNA test because it is predicated on more than one simple gene pair. Nonetheless, the future of breeding healthy dogs is made profoundly more “user friendly” with the available testing protocols for those who use them wisely.
“So, the tricky part, and I think the really hard part for people that as breeders are running these tests are for them to try and decide how to use that information in their breeding program,” Greer said. “… I see a lot of breeders who are so distraught about finding a genetic defect in their dog or in their line of dogs that they will throw out a whole line of dogs genetically. They will just stop breeding that whole line and it is narrowing and bottlenecking our gene pools even further than a lot of the breeds already are. So, we have to be really careful how we interpret and use those results.”
BREEDING DECISIONS
Greer goes on to discuss various health concerns and how those should apply to making breeding decisions.
“So, I tend to rank, personally, genetic diseases on a ranking of one, two and three, because you can’t treat them all the same,” Greer said. “So, things like an umbilical hernia, or an extra eyelash, you fix it once surgically, it is corrected. …the reality of it is those are not life-threatening diseases … Ranked two are things like allergies and thyroid disease, which require chronic medications. They always have to be on medication for those diseases if they have them. … And then ranked three are the things that are life-threatening, life-altering, life-changing diseases, and those are arthritic changes like hip dysplasia, seizures that are life-threatening, and, frankly, bad temperament in my opinion has the same categorization because some of those dogs have such bad temperaments that they bite people and that’s life-changing, life-altering and life-threatening. … I want to kind of frame it so people understand that not all not genetic diseases are the same, not all should be treated equally, and we have to really be thoughtful about how we use this information in breeding programs.”
The judicious and thoughtful use of health testing results and criteria in breeding healthy dogs presents almost a continuum of application in Greer’s experience. Potentially unhealthy dogs with no testing on one end and dogs with extensive testing but a potentially limited gene pool which may entrench diseases at the other end of the spectrum.
“…the Dandie Dinmonts, the Otterhounds, these people with small gene pools can serve as models for other breeds,” Greer said, “because even Labradors and Golden Retrievers are narrowed pools compared to what we have seen in the past. So, absolutely we need to be looking at these kinds of opportunities to perpetuate our genetics and not breed ourselves into such a bad corner that we end up with everything having a genetic disorder that is insurmountable, because some of these diseases are pretty serious and they become very ubiquitous in a breed.”
154 – Veterinary Voice with Dr. Marty Greer|C-Section Decisions

VETERINARY VOICE — C SECTIONS: WHEN, WHY AND HOW
DR. MARTY GREER, DVM, JD
Welcome to the debut of this exciting monthly feature here at PureDogTalk. Dr. Greer offers outstanding information on a variety of topics. She is a licensed veterinarian and attorney who specializes in reproductive issues at her clinic in Wisconsin.
PureDogTalk listeners are fortunate to have a front row seat for Dr. Greer’s knowledge, experience and compassion, now on a monthly basis.
CEASARIAN SECTIONS
We’re talking today about Ceasarian sections…. the when, why and how of a difficult and emotionally fraught, potentially emergency whelping situation.
“These are scary, tough decisions,” Greer said. “Breeders and veterinarians are often both conflicted.” We’ve provided a graphic in the show notes with excellent information on protocols and a decision making checklist.
Greer discusses the differences between working with your regular veterinarian and an emergency or referral clinic which may not be as familiar with you and your pet.
“It’s the middle of the night, you’re sleep deprived, your dog and puppies are in trouble,” Greer observed. “You don’t always get the response from (an emergency clinic) to promptly intervene.”
PROGESTERONE TIMING FOR PREVENTION
The best cure is prevention, Greer said. Plan ahead and be prepared. Her best suggestion is to do progesterone timing at the outset of the breeding. This timing will give breeders the best information as to exactly when a litter is due and take away a great deal of heart ache and hand wringing on the topic of whether a C section is required.
“Try to be prepared. Do progesterone timing,” Greer noted, “do a pregnancy confirmation ultrasound, do a puppy count xray. Have your whelping supplies together. Put gas in your car!”
Progesterone timing, while perhaps not necessary to get a bitch bred with a natural breeding, allows breeders to be organized and well prepared, according to Greer. If a bitch is bred every other day for a week, the breeder has NO idea when she ovulated. “And, you have no way to gauge if/when she might need a Csection,” Greer added.
Breeder can do reverse progesterone at the end of the pregnancy if needed, but Greer noted this becomes much more costly than simply pulling blood for progesterone at the beginning.
“Losing a litter is very expensive. It’s very emotional for everyone,” Greer said.
She also spends time talking about how and why to build a relationship with your veterinarian. Most particularly breeders are recommended to treat the veterinary practitioner well, bring goodies for the staff, establish mutual respect. It isn’t always easy to find a clinic willing to work with a breeder. Greer recommends taking good care of those folks!
Breeders can also mentor veterinary students in their homes. “Take (baby veterinarians) to events. Invite them to join you on whelp watch,” Greer said. “Its a great way to build a bridge. The more we can do to mentor, help them understand, the better off we are.”
Greer also encourages breeders to play fair with their vet clinic. “Pay for a consultation, sit down with the veterinarian, let them know ‘this is what I do, this is what I need.’ They will know you are sincere. You need to have face to face conversation. “
While we’ll have a checklist from Greer here on the show notes, some specific details from Greer for evaluating a bitch at home as to whether a situation constitutes an emergency.
GREEN MEANS GO!
Her primary commentary is “green means go.” If a breeder sees green vaginal discharge **prior to the delivery of the first puppy** it means the bitch has placental separation and at least one, if not more puppies, are in danger from a lack of oxygen.
A final note from Greer, is that 75 percent of C sections are due to a problem with the bitch i.e. breed specific issues, uterine inertia, the number of puppies and more. The remaining 25 percent of issues are caused by a puppy coming the wrong way, a log jam in delivery and ore in that vein.
Listen today for more absolutely critical, life saving information from an experienced practitioner.
EMERGENCY C SECTIONS QUESTIONS
Questions for evaluation of the bitch at home or at the hospital indicating the probable need for an Emergency C-Section:
- Has the bitch been in hard labor (abdominal pushing) over 2 hours on the first or 1 hour on subsequent pups?
- Did the bitch initially show good abdominal contractions and stop without producing a puppy?
- Is there is green vaginal discharge PRIOR to the delivery of the first puppy?
- Does the bitch seem distressed? Frantic? Sick? Weak or unable to stand? Tremoring? Repeated vomiting?
- Is this labor pattern different than her previous ones?
- Has the bitch been unwilling or unable to eat and/or drink for over 12 hours?
- Has WhelpWiseR indicated there is a problem with fetal heart rates (<160 BPM) or uterine contraction patterns?
- Have any pups been born dead?
- Did a previous radiograph or ultrasound suggest there could be a problem? (low heart rates on ultrasound or pups without visible heartbeats?) (Malpresented or very large pups)
- Is a pup palpated on vaginal examination and in an unusual position or not progressing through the birth?
- Did her temperature drop to 98 degrees and rise to normal (over 101.0) and stay there more than 4 hours?
- Has her pregnancy exceeded 63 days?
- Does she appear to have a very large or very small litter?
- Does she have a previous history of dystocia?
- Is she a breed at risk for maternal or fetal causes of dystocia?
- Does she have unexplained or unusual discharge from her eyes?
- Is she having weak or non-productive contractions with multiple puppies left?
- If oxytocin has been used (more later), has there been a minimal or no response?
- Does the breeder or veterinary staff member have a feeling that something is going wrong? Trust their intuition.
If the answer to any of these questions is yes, you very likely need to assess the bitch as soon as possible and advise your client that the bitch should proceed to emergency surgery unless you can immediately correct any cause for dystocia.